 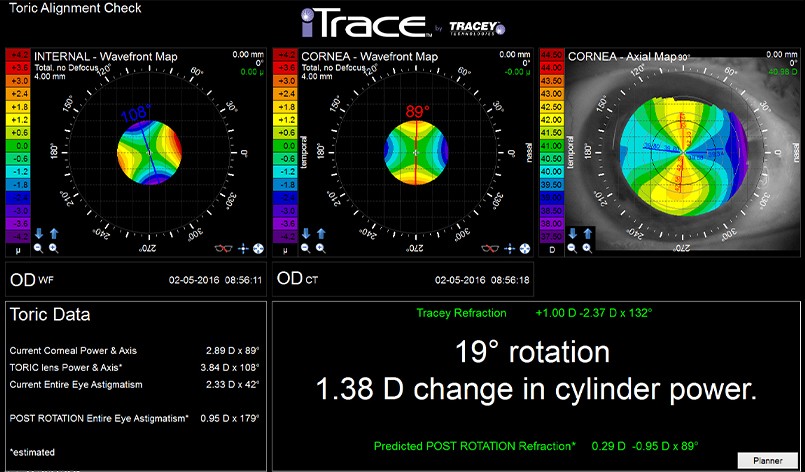 
Dry eye is the most common corneal condition that must be addressed prior to recommending premium IOLs. Here’s a look at the main corneal causes of dissatisfaction with premium IOLs postop: Figure 1 on page 17 shows an example of the cornea HOAs from corneal ectasia affecting the vision more than the internal HOAs. If we determine that the cornea is responsible for the loss in vision, we’ll focus on treating the corneal pathology first before recommending a lens implant. In this case, the corneal aberrations make up the majority of the total HOAs (which is from corneal ectasia s/p LASIK) and therefore cataract or lens exchange surgery wouldn’t be beneficial for this patient instead, the corneal aberrations should be addressed]. The internal aberrations are assumed to be from the natural lens or IOL. The iTrace separates the total HOAs of the eye into the corneal and internal aberrations. The image above shows the wavefront measurements of the eye and a combined placido disc image of the anterior corneal surface. We also use an RGP CL over-refraction in cases of irregular astigmatism and compare that to the manifest refraction if the RGP over-refraction improves the BCVA then we know the cornea is the source of poor vision.įigure 1. An easy way to determine if it’s a cornea or lens issue is by performing wavefront measurements (Tracey’s iTrace and Nidek’s OPD-III are common instruments available in the United States). By using monofocal IOLs we can provide our patients their best quality of vision possible.įirst, we determine if the vision loss is from corneal pathology or internally (i.e., the lens). If there are any findings on the anterior segment or dilated fundus exam that will limit the patient’s visual potential, we typically recommend monofocal IOLs with or without monovision. There are many reasons to avoid MF or even EDOF lenses in patients that have limited visual potential: (1) loss of contrast sensitivity from the IOL, (2) the perceived lack of value of a premium IOL if the patient is paying extra out-of-pocket and not achieving their best potential vision, (3) remove the confusion postoperatively as to the cause of decreased vision-i.e., is it the IOL or some other ocular pathology? In this article we’ll focus on the anterior segment/cornea conditions that can affect the outcomes of premium IOLs, namely ocular surface disease, Salzmann’s nodular degeneration, epithelial basement membrane dystrophy, Fuchs’ endothelial dystrophy and irregular astigmatism. 
To come to that decision, we evaluate the patient from front to back-from the ocular surface to macula-and address any findings with them preoperatively in order to avoid any mistrust or surprises postoperatively. S ince I started implanting premium IOLs in 2002, I’ve learned when to offer these lenses and when to avoid them. Artificial Intelligence for the Cornea SpecialistĭSO and Cultured Endothelial Cell Transplants: A Reviewīy Thomas John, MD, and Anny M.S. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
